
Full Mouth Reconstruction in the San Francisco Bay Area, CA
Serving the San Francisco Bay Area · Palo Alto · Menlo Park · Mountain View · Los Altos · Cupertino · Sunnyvale · San Jose · and all of Silicon Valley
Some patients come to Dr. Pai with a single cosmetic concern. Others arrive with a mouth that has been quietly deteriorating for years: worn teeth, a collapsing bite, chronic jaw pain, restorations that are failing one after another.
Full mouth reconstruction is for the second group. It is the most complex treatment in dentistry and is also the most life-changing. Dr. Nidhi Pai has been doing this work in the Bay Area for over 25 years.

What is full mouth reconstruction?
Full mouth reconstruction (also called full mouth restoration or full mouth rehabilitation) is the complete rebuilding of the teeth across both arches. It is different from a smile makeover in one important way: the primary problem is clinical, not cosmetic. The bite has collapsed. The teeth are structurally compromised. The damage is too widespread to fix tooth by tooth. Reconstruction addresses all of it in a coordinated plan.
Done well, patients stop waking up with headaches. They can eat foods they had quietly given up on. They stop covering their mouth when they laugh. And for the first time in years, they have a bite that actually feels stable.
It is not a single procedure. Depending on the case, it can combine crowns, veneers, implants, gum treatment, bite correction, and alignment therapy across multiple appointments over several months. The sequence matters enormously, which is why planning is where Dr. Pai spends the most time.
What to Expect
Full Mouth Reconstruction vs Smile Makeover
People sometimes use these terms interchangeably, and in practice they do overlap. But the distinction matters. A smile makeover starts from cosmetic goals: the teeth are healthy, the bite is stable, and the patient wants to change how their smile looks. A reconstruction starts from clinical necessity: the bite has been compromised, the teeth are breaking down, and restoring proper function is the first priority.
In Dr. Pai's experience, most reconstruction patients end up with both. The clinical problems are addressed in the correct order, and the aesthetic result follows from a foundation that is built to last. But the sequence is driven by function, not appearances. You cannot put veneers on a collapsing bite and expect them to hold. That is a lesson Dr. Pai learned early and applies to every case she takes on.
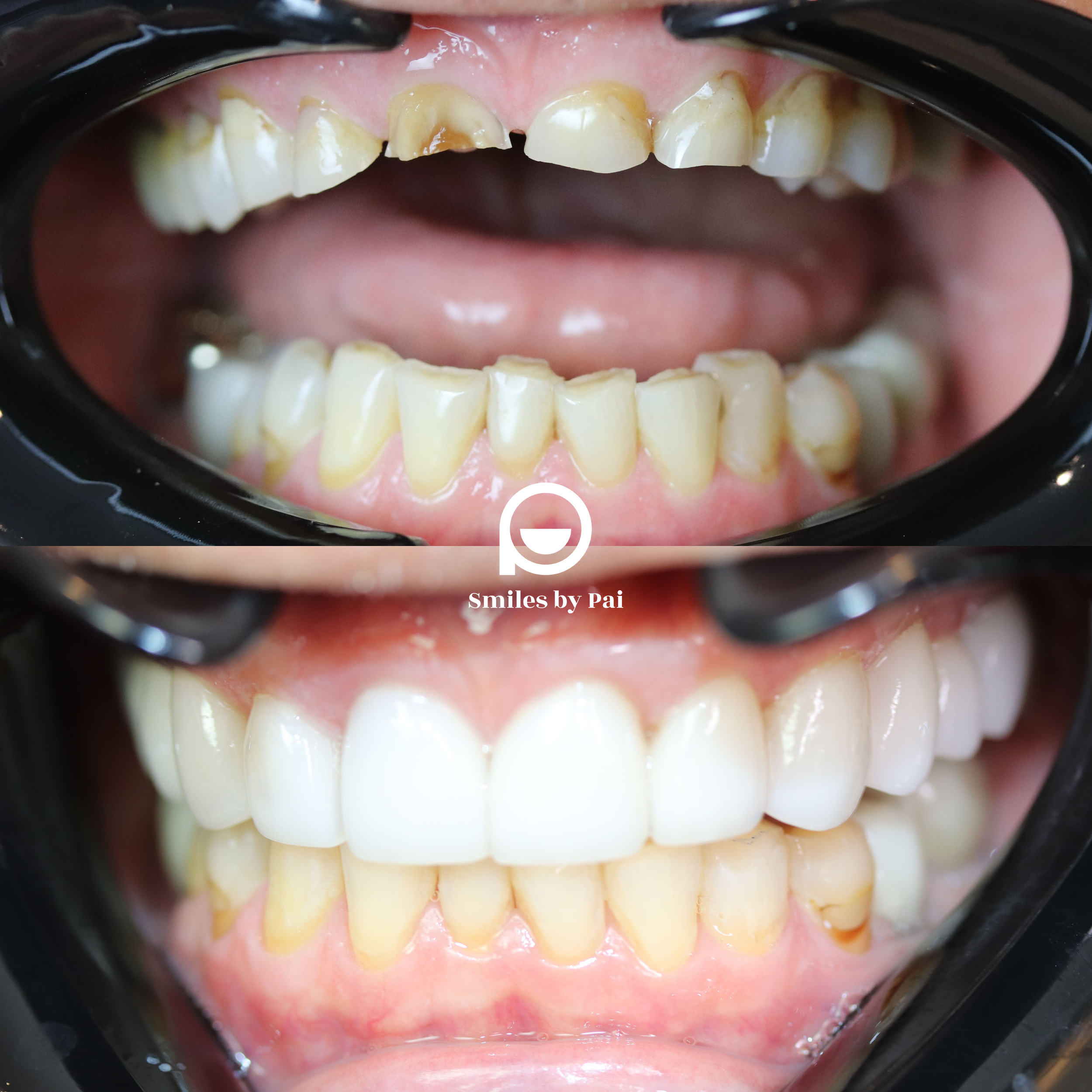
Extreme Smile Makeover:
Full Mouth Reconstruction with Nidhi Pai, DDS
Who Is a Candidate for Full Mouth Reconstruction?
Full mouth reconstruction is recommended when damage has spread across most of the mouth: through wear, decay, tooth loss, or some combination of all of those. The most common situations Dr. Pai sees:

Severe Tooth Grinding and Clenching
Bruxism (chronic grinding and clenching, often during sleep) is one of the most common causes of full mouth damage. Over years and decades, it wears teeth down to fractions of their original height, collapses the bite, strains the jaw joint and muscles, and can ultimately lead to tooth fracture and loss. Many patients do not know they grind until the damage is already extensive.
Enamel Erosion
Acid erosion from diet, acid reflux, or certain medications strips enamel from the tooth surface, leaving teeth sensitive, discolored, and structurally weakened. Once enamel is lost it cannot be regenerated, and when erosion is severe across multiple teeth, full reconstruction is often the only path to restoring both function and aesthetics.
Multiple Missing Teeth
When several teeth are missing: whether from injury, decay, or extraction: the remaining teeth shift, the bite collapses, and bone loss begins. Full mouth reconstruction replaces missing teeth with implants or supported restorations, restores the bite to its correct dimension, and prevents the cascade of problems that untreated tooth loss causes over time.
Failed or Aging Restorations
Crowns, bridges, and large fillings placed decades ago eventually wear out, fracture, or fail. When multiple restorations across the mouth are failing simultaneously, individual replacement is no longer the most effective approach. Full mouth reconstruction replaces everything at once, at a consistent standard, with a cohesive aesthetic result.
Bite Collapse and TMJ Problems
When the bite loses its correct vertical dimension: through grinding, tooth loss, or worn restorations: the jaw joint (TMJ) and surrounding muscles compensate. This leads to jaw pain, headaches, ear pain, neck tension, and difficulty chewing. Reconstruction re-establishes the correct bite height and alignment, resolving the downstream symptoms that patients often do not connect to their teeth.
Congenital or Developmental Conditions
Some patients are born with conditions that affect the number, size, or structure of their teeth: including amelogenesis imperfecta, dentinogenesis imperfecta, or simply the absence of multiple teeth. Full mouth reconstruction provides a comprehensive, sequenced plan rather than addressing each issue piecemeal over years.
Trauma and Injury
Accidents, falls, and sports injuries can cause extensive damage across multiple teeth simultaneously. When trauma affects the entire bite: not just one or two teeth, full mouth reconstruction restores everything in a coordinated plan that considers both the clinical repair and the long-term aesthetic result.
Severe Decay or Periodontal Disease
Advanced decay or periodontitis that has compromised the health and structure of most teeth in the mouth requires a comprehensive rebuild: treating the underlying disease first, then restoring the teeth to full function and appearance on a healthy foundation.
Procedures that may be a part of your plan
No two reconstruction plans are the same. What goes into yours depends entirely on what Dr. Pai finds at your clinical assessment. These are the procedures she draws on:
-
Full-coverage restorations that cap a damaged or structurally compromised tooth, restoring its strength, shape, and appearance. The primary workhorse of full mouth reconstruction when teeth are structurally intact but significantly damaged.
-
Ultra-thin ceramic shells for the front teeth, used when the underlying tooth structure is sound but the surface is worn, stained, or damaged. Dr. Pai often uses veneers for the aesthetic front teeth in combination with crowns on the functional back teeth.
-
Permanent replacement for missing teeth, placing a titanium root and custom crown that functions and looks exactly like a natural tooth. In full mouth reconstruction, implants often anchor the bite where natural teeth can no longer do so.
-
Precise adjustment of how the upper and lower teeth meet, establishing the correct vertical dimension and contact pattern before permanent restorations are placed. This is foundational to the entire reconstruction.
-
Sometimes teeth need to be repositioned before reconstruction can begin, particularly when misalignment is contributing to the bite problem or would compromise the outcome of restorations. Dr. Pai is a Top 1% Invisalign provider and often incorporates alignment as the first stage of a full reconstruction plan.
-
Gum disease must be fully treated before any restorative work begins. Healthy gum tissue is the foundation that every restoration rests on. Dr. Pai coordinates with periodontal specialists when the gum environment requires specialist intervention.
-
When the gumline is uneven, receded, or displaying too much tissue, gum work is incorporated to create the ideal frame for the reconstructed teeth. The gums and the teeth must work together aesthetically and clinically.
-
When implants are part of the plan and bone density is insufficient, bone grafting rebuilds the volume needed to support the implant post. Coordinated with Dr. Pai's oral surgery partners.
-
For cases where speed and efficiency matter, Dr. Pai's CEREC technology can fabricate certain crowns in a single appointment, with no temporaries and no second visit.
-
For patients whose reconstruction was driven by bruxism, a custom night guard is the final step. It protects everything that was just rebuilt from the same grinding forces that caused the original damage
Frequently Asked Questions About Full Mouth Reconstruction
-
It depends on what the case involves. A straightforward case covering both arches with crowns and no implants or preparatory work might be done in three to six months. A more involved case with implants, bone grafting, periodontal treatment, and Invisalign alignment could take a year or more. Dr. Pai gives a realistic timeline at your consultation after a proper clinical assessment. The two-month temporary phase alone is non-negotiable in complex cases, and that is part of why the results hold up.
-
Cases in the Bay Area typically range from $25,000 to $80,000 or more, depending on the number of teeth involved, the procedures required, and how complex the bite correction is. Dr. Pai provides an itemized treatment plan with full pricing before any work begins. She is also happy to discuss phasing the treatment over time for patients who need that flexibility. Financing options are available.
-
Less so than most patients expect. Procedures are done under local anesthesia. The temporary phase is usually comfortable once the bite settles, though some patients notice sensitivity or muscle fatigue while adapting to the new position, which is normal. Dr. Pai prepares patients thoroughly for what each stage involves, so there are no surprises. The most common thing patients say afterward is that it was easier than they thought it would be.
-
Many cases do involve specialist care at certain stages: oral surgeons for implant placement, periodontists for gum disease, orthodontists for alignment. Dr. Pai coordinates all of it through her Bay Area specialist network. Patients have one primary clinician throughout. Nobody gets sent off to figure out how the pieces fit together on their own.
-
Porcelain crowns and veneers typically last 15 to 25 years. Implants can last a lifetime. Longevity depends on the quality of the planning and materials, how stable the bite is, how well the patient maintains their oral hygiene, and whether bruxism patients wear their night guard consistently. Dr. Pai plans every reconstruction with a 20 to 30 year horizon. The decisions she makes at the planning stage are specifically intended to hold up over that kind of timeframe.
-
Yes. This is a significant clinical and financial commitment, and the right approach depends heavily on the experience and judgment of the treating dentist. Dr. Pai welcomes second-opinion consultations. She will tell you honestly what she sees, what she would recommend, and why, whether or not it matches what you have already been told.
-
Often yes, when those symptoms are coming from a collapsing bite or chronic bruxism. Re-establishing the correct bite height takes the compensatory load off the jaw muscles and joint, and many patients find the pain that has followed them for years starts to resolve during the temporary phase. Dr. Pai will assess whether your symptoms are bite-related at your consultation and give you a straight answer about what reconstruction is likely to change.
Schedule a Consultation
Tell Dr. Pai what you have been dealing with. She will take the time to look at everything properly and give you an honest picture of what is possible.


